WHO Declares Mpox an International Public Health Emergency, What Nurses Need To Know 2024
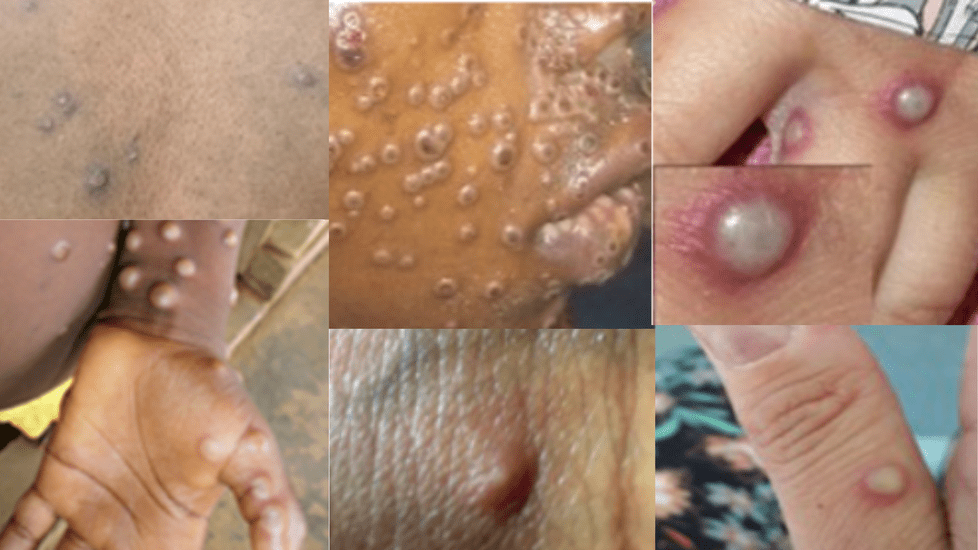
Image: CDC.gov
The World Health Organization (WHO) declared the recent Mpox outbreak a public health emergency of international concern in August 2024. Here’s what you need to know about this viral infection. According to the HHS.gov website,
- Africa Centres for Disease Control and Prevention (Africa CDC) declared the mpox clade I outbreak a Public Health Emergency of Continental Security.
- The World Health Organization (WHO) declared this outbreak a Public Health Emergency of International Concern.
- The United States will continue to work closely with African governments, Africa CDC and WHO to ensure an effective response to the current outbreak and to protect the health and lives of people of the region.
The HHS website states, "The risk to the general public in the United States from clade I mpox circulating in the DRC is very low, and there are no known cases in the United States at this time." According to the U.S. CDC Travel Health Notice released on August 7, 2024, travelers to DRC and neighboring countries should practice enhanced precautions.
What is Monkeypox?
Monkeypox (MPX) is a virus from the Orthopoxvirus genus of viruses. You will recognize related viruses, including:
- Variola (smallpox)
- Vaccinia (a poxvirus similar to smallpox but less dangerous)
- Monkeypox
- Cowpox
Scientists documented the first human cases of monkeypox in 1970. Since then, rare cases have been confined to central and western Africa. However, the Center for Disease Control and Prevention (CDC) now reports that 77 countries have confirmed MPX cases.
Source: CDC.gov
In the US, the CDC has reported 744 cases in 2024 in the United States and considers this to be low transmission of Mpox in 2024. There are currently no cases in the US. Watch the nationwide map and case count on the CDC’s website for updates. Also, review the trends report here.
There are two common clades (strains) that nurses should know. They are currently named after the region most commonly affected by the clade, but some experts suggest renaming them to reduce geographic stigma.
- Central African/Congo Basin monkeypox: causes more severe infection with around a 10% mortality rate.
- West African monkeypox: causes a milder infection with a mortality rate of around 1%; this is the only strain identified in the US cases.
This content used under license from "Ask Nurse Alice."
How is Monkeypox Transmitted?
The MPX virus is transmitted through direct contact with infected body fluids, skin lesions, or respiratory secretions. People can also become infected by touching bed linens or clothing used by someone with the virus.
Research suggests that airborne particulates can also spread the virus through prolonged face-to-face contact or intimate physical contact like kissing or sex. Routes of entry include oropharynx, nasopharynx, and intradermal.
Pregnant women who become infected may also transmit the virus to their babies.
A person is considered infectious from the onset of illness until all lesions have crusted over.
The virus can spread from human to human or from animal to human. Rodents and primates may be carriers. A monkeypox outbreak in 2003 started with infected animals that were shipped to Texas from Ghana. The incubation period for MPX is between 1–2 weeks and 21 days from exposure.
People with Increased Risk
According to the CDC,99% of cases were among men; among men with available information, 94% reported male-to-male sexual or close intimate contact during the 3 weeks before symptom onset. This pattern matches what we see globally. Health authorities worldwide say that reported MPX cases are overwhelmingly in men who have sex with men — disproportionately in those with multiple sex partners or who attend events where people have sex with strangers.
However, experts warn that the virus will likely spread to other groups. The first two pediatric cases in the US were confirmed last week.
Scientists say monkeypox is far less transmissible than the coronavirus that causes covid-19, which was also placed on the WHO’s highest alert level in January 2020.
What are common monkeypox symptoms?
The typical presentation for the MPX virus is flu-like. Individuals may experience symptoms including:
- Chills
- Fever
- Headache
- Lymphadenopathy
- Malaise and fatigue
- Myalgia
- Rash with fluid-filled pustules (“pox”) on the face, mouth, or body
- Severe pain
- Sore throat
Lymphadenopathy is significant in MPX infection because measles and chickenpox do not cause swollen lymph nodes. Therefore this sign is a key indicator for diagnosis.
Health officials also note that the most recent MPX cases involved genital rashes that could be mistaken for syphilis or herpes.
To date, there have been zero reported MPX deaths in the US.
Monkeypox Prevention
The public can prevent MPX spread by following these recommendations:
- Practice proper hand hygiene with soap and water
- Clean and disinfect high-traffic surfaces regularly
- Practice safe sex, including the use of condoms and dental dams
- Avoid contact with contaminated clothes or bedding
- Avoid contact with infected people
Nurses and other healthcare workers caring for infected patients or persons under investigation (PUIs) for MPX should wear the following PPE:
- Gloves
- Gown
- Goggles or face shield
- Particulate respirator mask (N95)
Healthcare facilities should have precautions in place to isolate persons with suspected infections.
Monkeypox Vaccines and Treatments
According to the CDC, there are currently two vaccines available for mpox in the US. Since MPX is related to the smallpox virus, the US has vaccines and antiviral drugs that can fight the virus. Yet, it is still hard to get a monkeypox treatment, and labs have limited testing capacity.
Vaccines are being used for prevention in high-risk individuals (such as healthcare workers treating MPX cases) and for post-exposure management. Vaccines must be given within four days of exposure for the best chance of preventing infection. They may limit disease severity if given within 4-14 days.
The WHO has said that mass vaccination is not recommended at this time. Instead, doctors should make treatment decisions by weighing risks and benefits on a case-by-case basis.
Here is a look at the three most common MPX treatments.
- JYNNEOS vaccine (Imvamune or Imvanex): The FDA has licensed the JYNNEOS vaccine to treat smallpox and monkeypox in people 18 years and older. It is administered in two subcutaneous injections, four weeks apart. According to the CDC, It is about 85% effective. However, there is a JYNNEOS shortage. As a result, manufacturers have ramped up production and expect almost 800,000 doses to be available for distribution by August.
- ACAM2000 vaccine: An older vaccine called ACAM2000 is approved for smallpox, and there is an ample supply. However, ACAM2000 contains live vaccinia virus. Hence, healthcare providers should not give it to people with the following conditions:
- weakened immune systems
- heart disease, some eye diseases
- certain skin conditions such as eczema or psoriasis
- Pregnancy
It can cause serious side effects.
Tecovirimat (Tpoxx) antiviral
Tpoxx, or tecovirimat, is an antiviral approved for orthopoxvirus-associated infections that can be used to treat MPX. Unfortunately, doctors have had trouble prescribing it. The CDC and FDA recently announced a new protocol to make it easier for doctors to get Tpoxx for their patients. The Expanded Access Investigational New Drug protocol (EA-IND) requires providers to consult with the CDC or their state/local health department to prescribe it.
Healthcare workers, military personnel, or other individuals who were previously vaccinated against monkeypox may still have some immunity against MPX.
Visit CDC.gov for updated information on Monkeypox
*This website is provided for educational and informational purposes only and does not constitute providing medical advice or professional services. The information provided should not be used for diagnosing or treating a health problem or disease.






