How To Draw Blood: A Step-By-Step Guide
This article has been reviewed by our panel of experienced registered nurses:
- Tyler Faust, MSN, RN
- Chaunie Brusie, BSN, RN
- Kathleen Gaines, MSN, RN, BA, CBC
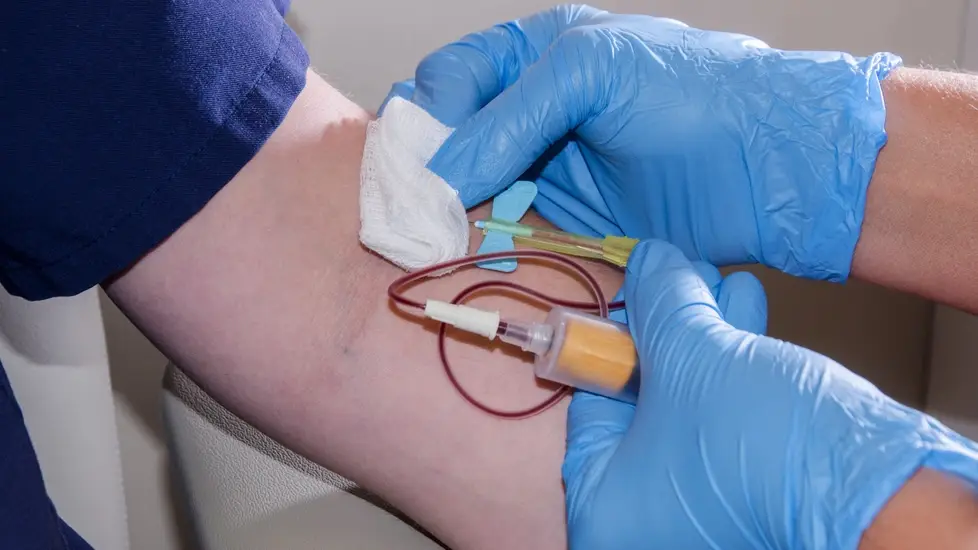

This article will take you through the basics of how to draw blood so you can understand the steps and current guidelines for best practice. Remember to check with your healthcare institution about specific policies and procedures regarding blood draws as well as any state regulations before performing any procedure.
Nurses Helping Nurses: Why You Can Trust Nurse.org
As the leading educational website for nurses by nurses, Nurse.org is committed to editorial integrity, medical accuracy, and data-driven analysis.
✔ Content written by 80+ licensed, practicing nurses who are experts in their respective specialties. Learn more about our nurse contributors.
✔ Medical and expert reviews by nurses for clinical accuracy and to ensure our content reflects the latest medical and nursing standards.
✔ Reputable sources from the World Health Organization (WHO), research institutions and associations, as well as academic, nursing, and medical journals. Learn more about our data resources.
How to Draw Blood
Drawing blood from a patient can be a daunting task, but it also is a necessity for nurses. Here are the basic steps to drawing blood:
- The first step is to discuss with the patient what you will be doing and why as well as gather all the needed supplies.
- Next, identify the vein that you will be using. The most common vein is the antecubital fossa; however, the median cephalic and median basilic veins are also used.
- Clean your hands via hand washing or hand sanitizer.
- Don gloves.
- Place a tourniquet and clean the area for 30 seconds with an alcohol wipe using a back-and-forth technique.
- Allow the area to dry for approximately one minute following cleansing the area.
- Pull the skin taut to anchor the vein.
- Insert the beveled needle at a 15 to 30-degree angle into the vessel.
- Once blood is seen in the tubing, connect the vacutainers or use a syringe to draw the needed amount.
- Properly label the tubes (at the bedside) and send them to the laboratory for analysis.
Step 1: Identify The Vein
The first step in drawing blood correctly is to identify the appropriate veins to puncture. For adult patients, the most common and first choice is the median cubital vein in the antecubital fossa. Commonly referred to as the antecubital or the AC it can be found in the crevice of the elbow between the median cephalic and the median basilic vein.
This is an extremely large vessel and, if stuck properly, can yield excellent blood results. Some healthcare settings may insert blood drawing peripheral intravenous catheters into this vessel for frequent blood draws.

For novice phlebotomists, this vein is the first choice because it is close to the skin’s surface and tends not to roll when punctured. Furthermore, it has a low risk of damaging surrounding nerves, arteries, and tendons versus other veins in the hands.
Learning the anatomy of the main veins and arteries in the body is essential to becoming competent in phlebotomy. If the AC has already been accessed, there are other great options for venipuncture.
Other commonly used veins include:
- Basilic vein
- Cephalic vein
At the end of the day, you will be most successful at a blood draw if you access the best vein. This will be the vein that you can feel or see most prominently. This will vary depending on your skill level and comfort level with blood draws.
Avoid Puncturing These Areas
While it is important to know the best veins to access, it’s also important to know which areas to avoid.
These areas include:
- Edematous sites (swollen sites filled with serous fluid)
- Scarred or burned areas
- Fistulas and grafts
- Hematomas
- From an IV cannula (unless permitted by your institution)
- Sites above an IV cannula in the same vessel
- Arm with PICC line
- Arm with a preexisting or current blood clot
- Arm on the side of a mastectomy
- Via an open wound or area of infection
- Arm in which blood is being transfused
- Arm on the side of a surgical procedure
Step 2: Gather Supplies
After identifying the site for the blood draw, gather the appropriate supplies needed. Some institutions have kits with all of the needed supplies, while others will require the nurses to gather them individually. An important tip - take extra supplies into the patient’s room in case you need to attempt a second venipuncture.
These supplies include:
- Evacuated Collection Tubes (tubes specific to labs ordered)
- Personal Protective Equipment (ie gloves)
- Appropriate blood-drawing needles
- Tourniquet
- Hand Sanitizer
- Alcohol swabs or Chlorhexidine wipes (CHG) for skin disinfection
- Laboratory specimen labels
- Gauze
- Blood transfer device
- Adhesive bandage/tape
- Laboratory forms
- Bio-hazard leak-proof transportation bags
- Puncture-resistant sharps container
Step 3: Venipuncture
After assembling the appropriate equipment, follow the next steps to perform a proper venipuncture. Once again, please be aware that these are only guidelines for blood draws and nurses should consult with the appropriate hospital personnel regarding performing this procedure on patients.
Additionally, these steps only apply to the adult and pediatric population and not neonates.
- Explain the procedure and reason for the blood draw to the patient.
- Identify the patient using two patient identifiers as mandated by JCAHO.
- Confirm the ordered tests and fill out the appropriate forms and labels.
- Check for any allergies or sensitivities with the patient regarding antiseptics, adhesives, or latex. True allergies should be identified on an allergy ID band, but sensitivities may not be reported at the time of patient admission.
- Position the patient and hyperextend the patient’s arm.
- Perform good hand hygiene and don appropriate PPE.
- Apply a tourniquet approximately 3-4 inches above the selected site. Closely monitor the arm to ensure that it is not applied too tight or for more than 1 minute. Reasons for concern would include numbness, tingling, change of color to blue or white, and/or extreme pain.
- Ask the patient to make a fist and not pump the hand. This is a common misconception - pumping the hand does not increase venous circulation.
- Prep the venipuncture site by cleansing the area with an alcohol prep pad for 30 seconds and allow to air dry for 60 seconds. Do not wave, fan, or blow on the area as this contaminates the area and leads to an increased risk for infection.
- Grab the patient’s lower arm (below the site of the puncture, never above) firmly to draw the skin taut and anchor the vein from rolling. Insert the needle at a 15 to 30-degree angle into the vessel.

- If properly inserted, blood should flash into the catheter. If this does not happen, then the needle has either not punctured the vein or the needle went through the vessel.
- If you do not get a flash of blood into the catheter, you can manipulate the catheter; however, do not entirely remove the catheter and re-stick using the same needle.
- Attach the needed tubes or syringes to remove the proper volume of blood. Remove the tourniquet as the last amount of blood is drawn.
- Remove the needle from the patient’s arm and press down on the vessel with gauze.
- Dispose of contaminated materials and needles in the designated hospital-approved containers.
- Label appropriate tubes at the bedside and place them into transport bags.
- Invert the tubes properly (depending on the type of tube).
- Deliver blood specimens to the laboratory promptly. If the blood is not delivered in a timely manner, it can cause hemolysis and skew the lab results.
Don’t be discouraged if at first, you don’t access the vein. Venipuncture is a skill that takes time and practice to master. Always remember to ask for help from seasoned nurses and seize opportunities to practice your skills.
The World Health Organization's Blood Draw Guidelines
The World Health Organization’s (WHO) best practice guidelines for blood draws include the following:
- Planning ahead
- Using an appropriate location
- Quality control
The overall purpose of establishing the guidelines is to,
- Improve knowledge and awareness of the risks associated with phlebotomy among all health workers involved in the practice
- Increase safe practices and reduce blood-borne virus exposure and transmission
- Improve patient confidence and comfort
- Improve the quality of laboratory tests
The WHO has set forth the following standards of patient care for hospitals to adhere by:
- Availability of appropriate supplies and protective equipment
- Availability of post-exposure prophylaxis (PEP)
- Avoidance of contaminated phlebotomy equipment
- Appropriate training in phlebotomy
- Cooperation on the part of patients
- Quality of laboratory sampling
They also identify dangerous and unsafe practices for blood draws including,
- Recapping used needles using two hands
- Recapping and disassembling vacuum-containing tubes and holders
- Reusing tourniquets and vacuum-tube holders that may be contaminated with bacteria and sometimes blood
- Working alone with confused or disoriented patients who may move unexpectedly contributes to needle sticks
>> Related: Arterial Blood Gases (ABGs) Explained
Things Nurses Should Know About Drawing Blood
For nurses to be successful when drawing blood, there are several key things they must know, including,
- Proper technique
- Proper safety standards to avoid a needle stick
- Vein placement in the arms
- Troubleshooting blood draws
- The rationale for blood draws
Blood Draw Best Practices
The WHO has best practices that are key to preventing infection and being successful during blood draws. Furthermore, they protect the nurse or healthcare professional from a potential needle stick.
Best practices in phlebotomy involve the following factors:
- planning ahead
- using an appropriate location
- quality control
- standards for quality care for patients and health workers, including
- availability of appropriate supplies and protective equipment
- availability of post-exposure prophylaxis (PEP)
- avoidance of contaminated phlebotomy equipment
- appropriate training in phlebotomy
- cooperation on the part of patients
- quality of laboratory sampling
Why Nurses Need to Learn How to Draw Blood
Obtaining blood samples, either via a venous stick or from a central line, is a critical nursing skill. Phlebotomy is essential for a variety of medical diagnoses, procedures, and tests. Without proper specimens, unhelpful or even harmful medical treatment could happen. Most nursing schools do not teach this skill due to legality issues. Students should study venipuncture in books and watch licensed nurses in clinical settings perform this task. In doing so, this will enable students to learn the basics prior to graduation.
Even though most hospitals do have phlebotomy teams, it is still critical for nurses to learn these skills in order to provide the best patient care. In fact, the majority of intensive care units require their nurses to possess these skills. Phlebotomy teams generally only make rounds at specific times in hospital settings; therefore, if a lab test is ordered immediately, it could be the responsibility of the nursing staff to draw the specimen.
FAQs
*This website is provided for educational and informational purposes only and does not constitute providing medical advice or professional services. The information provided should not be used for diagnosing or treating a health problem or disease.
Student Nurse

