27% of Nurses Were Physically Assaulted in 2025; Most Didn't Report It (Survey)

- 27% of nurses were physically assaulted at work in the past 12 months — hit, kicked, pushed, bitten, or grabbed — and 52% experienced verbal threats or aggressive language.
- Of nurses who had a workplace incident, only 54% formally reported it. The most common reason for not reporting: they didn't believe anything would change.
- Among nurses who did report, the most common outcome was no action taken. Fewer than 1 in 10 said they felt supported by leadership afterward.

One of the most disturbing findings in Nurse.org's 2026 State of Nursing Survey isn't the statistic itself — it's what nurses told us about what happens after.
More than half of the 2,090 nurses in our survey reported experiencing verbal threats or aggressive language at work in the past 12 months. More than 1 in 4 — 27% — were physically assaulted. Hit, kicked, pushed, bitten, or grabbed by patients, visitors, or others in their workplace.
And of those who experienced an incident and reported it to their employer, the most common outcome — by a significant margin — was that nothing happened.
Not a policy change. Not a consequence for the person who attacked them. Not even a conversation that felt supportive. Just silence, and then back to the next shift.
"I have been assaulted many times working on an inpatient adolescent psychiatric unit," one nurse wrote in the comments section of our survey. "No changes have been made to make our work environment safe. Management is full of empty promises. There is a complete lack of understanding regarding secondary trauma that affects many nurses and those working in healthcare."
That response captures something that shows up throughout our data: a workforce that has largely stopped expecting protection, because experience has taught them that reporting is an exercise in futility, and that the system designed to keep them safe has, in many cases, failed them repeatedly.
The Numbers
Workplace violence in nursing is not a new problem. The U.S. Bureau of Labor Statistics has documented for years that healthcare workers are roughly five times more likely to experience workplace violence than workers in other industries.
In our 2026 survey, among 2,090 nurses:
- 52% experienced verbal threats or aggressive language
- 27% were physically assaulted
- 10% experienced sexual harassment or unwanted sexual contact
- 4% faced a threat involving a weapon
- 4% reported stalking or harassment outside of work related to their job
To be clear: these are not near misses or uncomfortable interactions. Physical assault means a nurse was hit, kicked, pushed, bitten, or grabbed. More than 1 in 4 nurses in our survey experienced that in a single year.
The safety perception data underscores the cumulative effect. 34% of nurses say they do not feel safe from violence in their workplace.
The Specialties Where Violence Is Most Common
Workplace violence is not evenly distributed across nursing. Some specialties carry a disproportionate burden, and the data from our survey reflects that clearly.
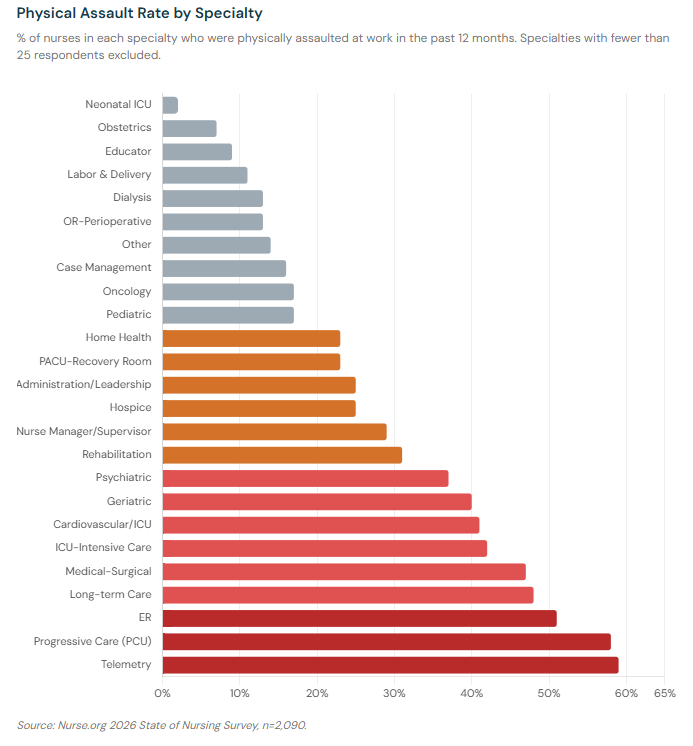
The range is striking. Nearly 3 in 5 telemetry nurses (59%) and progressive care nurses (58%) were physically assaulted in the past year. More than half of ER nurses (51%) say the same. At the other end, just 2% of NICU nurses and 7% of obstetrics nurses reported a physical assault — a reminder that specialty matters enormously when it comes to physical risk.
Verbal threats tell a similar story. 84% of ER nurses reported experiencing verbal threats or aggressive language in the past year — the highest of any specialty. Psychiatric nurses (76%), telemetry nurses (75%), and medical-surgical nurses (67%) also reported rates far above average.
The sense of unsafety follows the same pattern. 69% of ER nurses say they do not feel safe from violence in their workplace. Nearly two-thirds of psychiatric nurses (63%) say the same. Among progressive care nurses, 58% feel unsafe.
The age pattern in our data is also worth noting. Younger nurses carry higher assault rates: 37% of nurses aged 25–29 were physically assaulted, compared to 20% of nurses 65 and older. This likely reflects both specialty distribution and the reality that newer nurses are often assigned to higher-acuity, higher-volume settings.
The Reporting Problem
Of the 1,204 nurses in our survey who experienced at least one workplace incident, only 54% formally reported it to their employer.
The rest made a calculation — and in most cases, they calculated that reporting wasn't worth it.
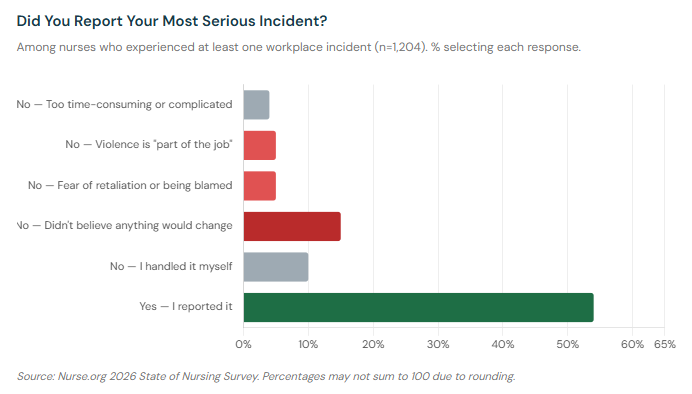
That last category — accepting violence as part of the job — may be the most concerning. When nurses absorb assault as a professional expectation, when it becomes so normalized that it doesn't feel worth documenting, the true scale of the problem becomes essentially unmeasurable.
"Violence in the workplace from patients and family members has become too mainstream with minimal consequences," one nurse wrote in our survey. "The attitudes and expectations from them post-COVID have skyrocketed for the worse. I feel this is a big reason why nurses are leaving the profession in droves and why there aren't as many coming in. We are tired of being verbal and physical punching bags and the consequences should be substantially worse than the proverbial slap on the wrist."
Another described the dynamic from inside a long-term care setting: "I started in healthcare at the age of 16 and since COVID the job has never been close to what it was when I began. I've been verbally abused, physically abused, and touched inappropriately. When you report these things time and time again it's swept under the rug."
The fear of retaliation is real and documented. One nurse wrote: "Reported unsafe conduct to no avail — retaliation from management." Another described a manager who, after a nurse reported being verbally abused by a patient's family member, went downstairs and bought lunch for that family rather than addressing the behavior.
"I told a manager and he said, 'So you don't care about your patients?' It took a lot of courage to get help. Now I feel guilty."
When Nurses Do File a Report
Among the 653 nurses in our survey who reported an incident to their employer, the outcomes were largely discouraging.
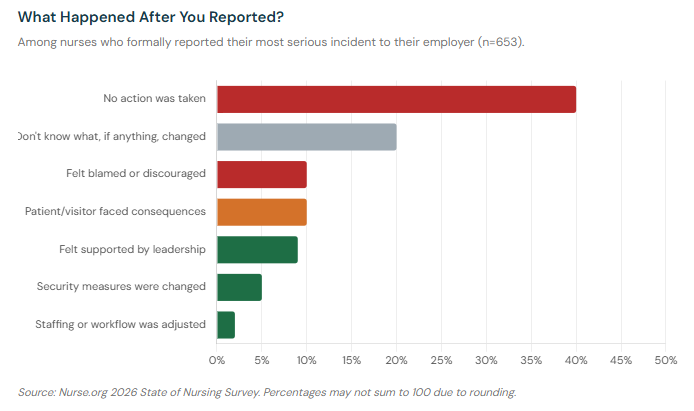
The single most common outcome — reported by 40% of nurses who came forward — was that no action was taken. Another 20% said they didn't know what, if anything, changed. Ten percent said they felt blamed or discouraged after reporting.
Only 9% of nurses who reported — fewer than 1 in 10 — said they felt supported by leadership after coming forward. Just 5% said security measures were changed as a result. Only 2% said staffing or workflow was adjusted.
"Nursing is not what it was in 1982 when I started," one nurse wrote. "When something happens, it is always the staff's fault. Nothing done. If it was towards a resident, something is done — as it should be. If anyone else is hit, kicked, etc., like a police officer or EMT, it is a felony. But not a nurse."
That last observation points to a genuine legal gap. A nurse in one state may have no more protection from assault than a retail worker, while the same attack on a flight attendant would trigger federal prosecution. The bipartisan Save Healthcare Workers Act (S.1600/H.R.3178), introduced in the Senate by Senators Angus King and Cindy Hyde-Smith in May 2025, would establish the first federal criminal penalties for assaulting hospital employees — giving healthcare workers the same protections that currently exist for airline and airport workers.
One nurse in our survey called for exactly this kind of action: "Workplace violence needs a nationwide zero tolerance. Too many states are soft on violence. This is why the federal SAVE the HEALTHCARE WORKERS ACT needs to be passed and signed by the President."
In Their Own Words
The numbers tell part of the story. The comments section of our survey tells the rest. What came back, again and again, was a description of violence that is routine, normalized, inadequately responded to, and quietly driving people out of the profession.
- "Post-pandemic, bedside nursing has become absolutely horrific. We as nurses are not respected — we are blamed, assaulted, threatened, spoken down to, and treated like garbage by patients, doctors, and our own managers."
- "Abuse comes in all forms. Unfortunately, I've experienced it not only from patients but fellow nursing staff at most of the jobs I've worked in. It's what sent me into traveling — although I still experience workplace violence, especially at the hands of charge nurses in California. I only have to ride out 13 weeks at those places as opposed to being staff and being abused for years at a time."
- "There was a time when nurses were praised for their sacrifice, time, and knowledge. Now we are the working mules of the hospital. We are the first staff member the patient sees, the last, the one who spends the most time with them — and with that, the most at risk for violence. There is no bedside protection if we defend ourselves."
- "I have never been so abused by family members and patients in my life. They have so severely abused me verbally and physically that I now need costly therapy and medication for severe anxiety. My depression is affecting my family and my quality of life."
What Needs to Change
Nurses in our survey were not short on ideas. When asked what would help, the same themes came up repeatedly: zero-tolerance policies with real consequences, staffing levels that allow for safer patient management, stronger legal protections, and institutional cultures that stop treating violence as an occupational hazard nurses are simply expected to absorb.
"Love helping patients but the environment is not safe when patients are not held accountable for threatening and assaulting staff," one nurse wrote. "Need zero tolerance policies with police support if charges are pressed."
"We need stronger policies around workplace violence and incivility," another wrote. "Not just signs on a wall."
The American Nurses Association has long maintained that workplace violence is not an inevitable part of nursing — that it is preventable, and that employers have a legal and ethical obligation to protect their staff. The Joint Commission has issued requirements for accredited organizations to develop workplace violence prevention programs. OSHA has published guidelines for healthcare settings. The tools and frameworks exist.
What is missing, nurses tell us, is the institutional will to use them — and the legal infrastructure to make consequences real and consistent.
The data in this survey is one step toward making the true scale of this problem visible. Nurses have been clear about what they need: consequences that match the severity of the offense, staffing levels that reduce risk, and employers who treat their safety as a priority rather than a liability. None of that is out of reach. What's required is the will to act on it.
This article is part of Nurse.org's ongoing coverage of the 2026 State of Nursing Survey. If you are a nurse experiencing workplace violence, the Emergency Nurses Association and the American Nurses Association both maintain resources and advocacy tools on this issue.
Nurse.org Annual State of Nursing Survey

