43% of Nurses Want to Leave the Bedside; Most Can't Afford To (Survey)

- 43% of nurses say they are likely to leave the bedside in the next year — up from 38% in 2025 — and 23% say they are likely to leave nursing entirely, up from 15% a year ago.
- Financial necessity is now the most common reason nurses stay at the bedside, cited by 41% of respondents — up from 35% in 2025 — outranking both commitment to patient care and personal satisfaction.
- Among nurses who want to leave but can't, the top barriers are financial constraints, lack of alternative job opportunities, and fear of change — not a belief that conditions will improve.

In Nurse.org's 2026 State of Nursing Survey, we asked nurses what is keeping them at the bedside despite any potential desire to leave. The most common answer — selected by 41% of nurses — was financial necessity.
Not commitment to patients, though that appeared too. Not love of the work, though that also showed up. The single most frequently cited reason nurses are staying at the bedside in 2026 is that they cannot afford to leave.
That number deserves to sit on its own for a moment. Because a workforce held in place primarily by financial constraint is not a stable workforce. It is a workforce under accumulating pressure, waiting for the moment the math changes.
The Scale of the Problem
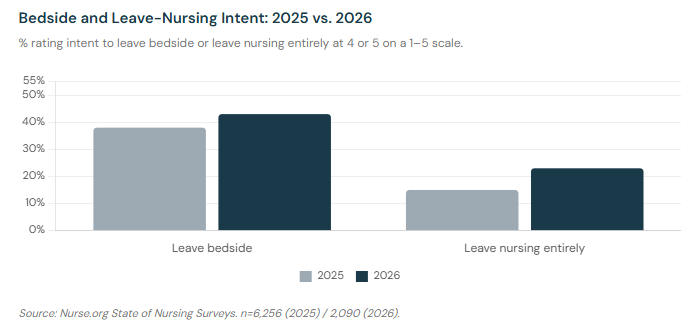
43% of nurses in our survey say they are likely to leave the bedside within the next year — rating their intent a 4 or 5 on a 1–5 scale. That is nearly one in two bedside nurses. And 23% say they are likely to leave the nursing profession entirely.
- 43% likely to leave the bedside in the next year
- 23% likely to leave nursing entirely in the next year
- 41% say financial necessity is keeping them at the bedside
The 2026 "leave the bedside" figure — 43% — is up from 38% in our 2025 survey. The "leave nursing entirely" figure climbed from 15% to 23% in the same period. Both represent meaningful increases in a single year, and both are moving in the wrong direction.
This is not a new problem in shape, only in degree. NCSBN's 2024 National Nursing Workforce Study found that 39.9% of RNs reported intent to leave the workforce or retire within the next five years, with stress and burnout identified as the leading reason beyond retirement. What our data captures is the deterioration happening right now — bedside intent-to-leave rising by five percentage points in a single year, and leave-nursing-entirely intent rising by eight.
Who Is Most Likely to Leave
The intent to leave the bedside is not evenly distributed. It clusters in predictable places: high-violence specialties, low-satisfaction units, and nurses at both ends of the age spectrum.
By specialty
Case management nurses had the highest "leave the bedside" intent at 71% — but this likely reflects career transitions rather than distress, since case managers frequently move to insurance, utilization review, or administrative roles. Among acute bedside specialties, psychiatric nurses (47%), oncology nurses (47%), and medical-surgical nurses (45%) show the highest intention to "leave the bedside." ER nurses are at 45%. Geriatric nurses, despite their low satisfaction scores, show lower intent to "leave the bedside" (34%) — which may reflect fewer available alternatives and the trapping effect of financial constraints described elsewhere in this article.
By age
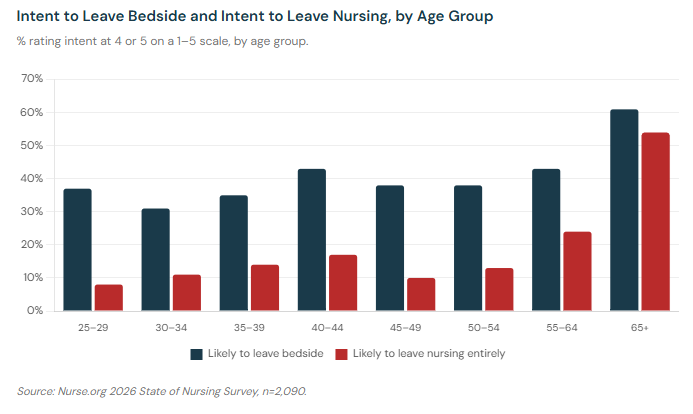
The age breakdown tells two different stories occupying the same statistic. Among nurses 65 and older, 61% say they are likely to "leave the bedside" — but most of those nurses are planning retirement, not fleeing poor conditions. Among nurses aged 40–44, 43% say they are likely to "leave the bedside," and only 17% say they are likely to "leave nursing entirely," which suggests they are planning lateral moves within the profession rather than exits from it.
The more concerning group is the middle of the age distribution. Nurses aged 35–54 — career-stage professionals with significant clinical experience, mortgage obligations, and families — show intent to "leave the bedside" at rates of 35–43%. These are not nurses who are retiring; these are nurses who are burning out.
By satisfaction
Among the least satisfied nurses in our survey — those rating their current job a 1 out of 5 — 68% say they are likely to "leave the bedside" and 40% say they are likely to "leave nursing entirely." Only 22% of these nurses would recommend a nursing career to a friend or family member. Only 41% say they feel safe in their workplace. And 54% cannot cover an unexpected $1,000 emergency without going into debt.
The picture that emerges from the least-satisfied nurses is one of compound crisis: low pay, high violence exposure, eroded safety, and a job that no longer pays enough to provide financial security — yet a job they feel they cannot leave. One nurse in this group wrote: "The nursing profession enjoyment has significantly decreased. It's a sad state when we are forced to think about finances over the care of the patients."
What Is Keeping Nurses at the Bedside
The question we asked — "What factors have kept you at the bedside, despite your potential desire to leave?" — produced answers that are worth examining carefully. Financial necessity led at 41%, but the full list reveals a workforce held in place by a complicated mix of obligation, loyalty, inertia, and love of work.
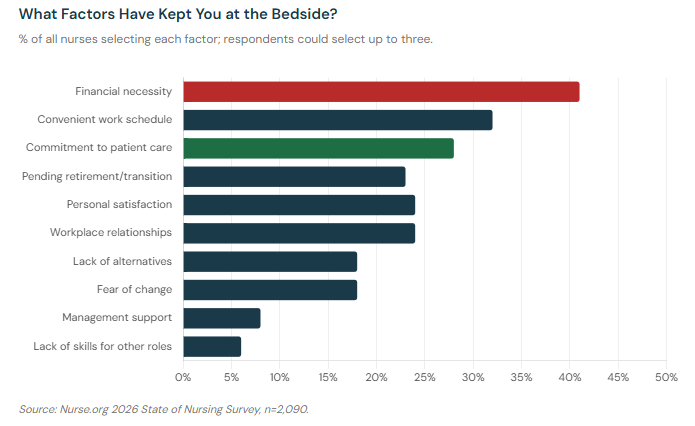
Financial necessity leads the list at 41% of all nurses. That figure is striking on its own — four in ten nurses say the primary reason they are still at the bedside is that they cannot afford to leave. That tracks directly with the financial stress data published in our article: 55% of Nurses Got Small Raises in 2025—Many Can't Cover a $1,000 Emergency. In that article, we discuss how 37% of nurses cannot cover a $1,000 emergency without debt, and 37% are working extra shifts due to financial pressure. Nurses are not just staying at the bedside because it pays — they are staying because they have no financial margin to do otherwise.
Commitment to patient care and personal satisfaction — the answers you might hope would lead — appear at 28% and 24% respectively. These figures are not small. Nearly three in ten nurses say that loyalty to their patients is part of what keeps them at the bedside. But the fact that financial necessity outranks both by a significant margin is meaningful.
Among nurses who specifically said they want to leave the bedside — those rating their leave intent 4 or 5 — the picture sharpens further. For this group, the top reasons for staying are financial necessity (38%), pending retirement or transition plans (30%), and lack of alternative job opportunities (21%). Commitment to patient care drops to fourth. These are nurses staying at the bedside because they feel they have no other option — not because the job is fulfilling their purpose.
20% of nurses — roughly 1 in 5 — cannot cover a $1,000 emergency AND are not likely to leave the bedside, suggesting financial constraint is directly limiting their options.
"My current position has me trapped," one float nurse wrote. "I cannot work in any of the units as a core nurse (units that I am currently working in as a float RN) without going back to working nights again. I have been a nurse at the same facility for 25 years, and in this current position as a float RN for over 20 years. My only option now is to leave my 25 years of seniority/benefits that I have established, and go to another facility, or stick it out until I retire (another 10+ years)."
Another nurse: "Although bedside nursing has fulfilling moments, staffing ratios and salaries not commensurate with inflation — and the lack of overtime availability as a result of hospitals trying to save money — cause nurses to need a second job or a job with an agency. And agencies are not paying well either when you calculate housing costs away from home."
Where the Ones Who Are Leaving Are Going
When asked what job they would most likely pursue if leaving the bedside, 20% of all nurses named retirement or stopping work entirely. Among those planning to stay in nursing, telehealth (9%) and nurse educator roles (9%) were the top choices, followed by case management (7%), nurse administrator (4%), and public health nursing (4%).
When asked about their plans if leaving nursing entirely, 54% of all nurses said they don't plan to leave, and 19% said they plan to retire or stop working. Another 16% said they want to stay in healthcare but get away from the bedside, and 4% said they want to go back to school for a career change. The remaining 7% named roles outside traditional nursing: pharmaceutical sales, physical therapy, legal nurse consulting, healthcare recruiting, etc.
The pattern that emerges is not of nurses fleeing healthcare — it is of nurses trying to stay in nursing while escaping the bedside conditions that are making them unwell. Telehealth, education, and case management are all paths that preserve the professional identity while removing the physical and psychological demands of direct acute care. They are, in many ways, the release valve for a workforce that has nowhere else to go inside its own profession.
A 2025 study published in JAMA Network Open surveyed over 4,000 nurses who had left hospital employment and found that roughly two-thirds said they would consider returning — if conditions improved. The three things they named most often: adequate staffing, scheduling flexibility, and better pay. None of those is a radical ask. All of them remain unmet in most institutions.
The Nurses Who Are Still There for the Right Reasons
It would be incomplete to tell only the story of financial entrapment. The data also contains nurses who are staying for exactly the reasons nursing is supposed to attract people — and who are doing so with their eyes open.
68% of nurses in our survey say they are happy about their decision to join the nursing profession. 47% would recommend a nursing career to a friend or family member. These are not the numbers of a profession that has lost its purpose. They are the numbers of a profession whose people still believe in the work, even when the work is breaking them.
Among nurses who stay at the bedside out of commitment to patient care, that commitment tends to produce better outcomes on nearly every satisfaction metric. These nurses report higher job satisfaction, stronger sense of professional identity, and greater willingness to recommend the career. They are staying not because they have no choice but because the job still means something to them. Protecting that group — the nurses who are there for the right reasons — is a worthwhile retention goal on its own.
"Nursing is hard work and definitely a labor of love," one nurse wrote. "It's sometimes hard to go to work when you feel awful, but you go anyway because you don't want to leave your coworkers short or knowing that patient care will suffer due to insufficient staffing. It’s not up to the individual to make sure the department/unit is staffed but often as nurses we take that responsibility on and feel guilty for not being there even when our bodies are telling us we shouldn’t be."
That last sentence is worth noting. The burden of retention should not fall on individual nurses willing themselves to stay. It should fall on institutions willing to create conditions where nurses are retained by something other than debt and fear of change.
In Their Own Words
The comments left by nurses in our survey on this topic were among the most direct in the survey. Here are voices from nurses navigating the tension between why they chose nursing and whether they can afford to leave it.
- "I feel very satisfied with the work that I do and the people that I save. However, I don't see myself staying in the profession for much too long. My opinions and decisions are made because of the work environments I have been a part of, and those have not been ideal at all."
- "The nursing profession has gone considerably downhill since I graduated in 2011. I left the bedside in 2022 and will never go back. I work from home and will work any job other than bedside nursing for the rest of my nursing career."
- "Nurses wouldn't be leaving the bedside if they felt more supported from leadership and administration. Staffing is purposely kept low, causing burnout to increase. You're penalized for calling out if you feel burnout or your body is worn down. Being forced to come in while sick and wear a mask to take care of immunocompromised patients shouldn't be allowed."
- "I fear for the younger nurses coming on. These kids are walking into a pressure cooker situation that's not getting better. When new nurses ask me for advice, I tell them to 'find a niche.' A place where they have some autonomy and control. I tell them to stay away from bedside care if they want to work as a nurse for any length of time."
- "I transitioned from the ED after 29 years to an ambulatory care setting last year after the hospital I worked for closed. I think the move helped to save my life and my mental health. I wish more nurses would consider switching things up to thrive in the work environment instead of just survive."
- "Nursing/healthcare has changed so much in the past 33 years. I don't feel comfortable encouraging people to go into healthcare unless they are extremely passionate about it or feel a 'calling.' Nursing is not just a paycheck. It is the heart and soul of healthcare. We are there through the good and the bad. I am currently a school nurse, biding my time until retirement."
That last phrase — "biding my time" — carries the essential tension. It is not the language of someone who left. It is the language of someone who stayed — and is counting the days.
The question worth asking is not only why nurses are leaving. It is what it costs to keep them — to the nurses, to the patients they care for, and to a healthcare system built on the assumption that clinical workers will absorb whatever it demands of them, indefinitely, because they have nowhere else to go.
This article is part of Nurse.org's ongoing coverage of the 2026 State of Nursing Survey.


