55% of Nurses Got Small Raises in 2025—Many Can't Cover a $1,000 Emergency (Survey)

- 55% of nurses received a pay increase last year, but for most it was just 1–5% — and 37% still couldn't cover an unexpected $1,000 expense without going into debt.
- 37% of nurses worked extra shifts or overtime due to financial stress in the past 12 months. Among those who took a second job specifically because of financial pressure, half still couldn't cover the $1,000 emergency.
- As educational debt increases, so does regret: 91% of nurses who carried no debt say their nursing education was worth it. Among those who carried more than $150,000 in debt, only 61% feel the same way.

More than half of nurses in Nurse.org's 2026 State of Nursing Survey — 55% — said their compensation went up over the past year. That sounds like progress. But look one question further, and the picture becomes more complicated.
37% of those same nurses say they could not cover an unexpected $1,000 expense without going into debt. 26% say their income barely covers or doesn't cover their essential monthly expenses at all. And 37% said financial stress pushed them to work extra shifts or overtime in the past 12 months — not because they wanted to, but because they had to.
The Gap Between Raises and Reality
When nurses say their pay increased, what does that actually mean? In our survey, 44% of nurses said their compensation rose by 1–5% over the past year. Another 6% saw increases of 6–10%, and just 4% saw increases above 10%. More than a third — 34% — saw no change at all, and 11% saw their pay actually decrease.
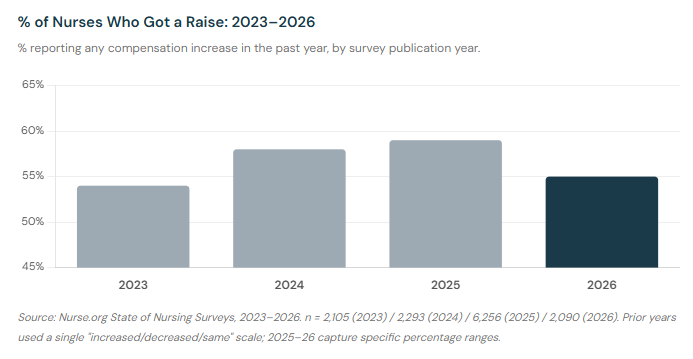
The raises nurses are receiving are modest. SullivanCotter's 2024 RN compensation survey found the median pay increase for registered nurses was 3–4% nationally, with regional variation — roughly in line with what our survey respondents reported.
The problem is that a 1–5% raise doesn't go very far when the cost of living has risen sharply in recent years. Healthcare insurance premiums, housing costs, and everyday expenses have all outpaced modest wage gains for many workers. "We are asked to take on more responsibility, yet we get raises that don't cover the cost of living," one nurse in our survey wrote, "including rising premiums cost for healthcare insurance and out-of-reach deductibles."
Another put it more bluntly: "The raise given to us this year does not even cover the increased costs of our benefits, much less keep up with the cost of living increase."
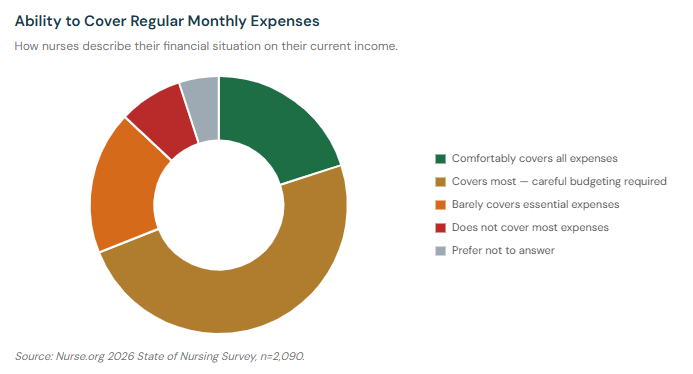
The $1,000 emergency test is a widely used measure of financial resilience. In our survey, 37% of nurses said they couldn't pass it. Notably, even among nurses who received a pay increase, 33% still couldn't cover a $1,000 emergency — suggesting that for many, raises are simply treading water against rising costs rather than building financial security.
Who Is Struggling Most
Financial strain in nursing is not evenly distributed. It tracks closely with salary band, education level, and — perhaps most strikingly — career stage.
The salary data tells a clear story at both ends. Among nurses earning over $120,000 a year, 63% can cover an unexpected $1,000 expense without debt, and 41% describe themselves as financially comfortable. Among nurses earning $60,000–$70,000 — a bracket that includes a significant share of the workforce — only 33% could cover the emergency, and 48% say they cannot.
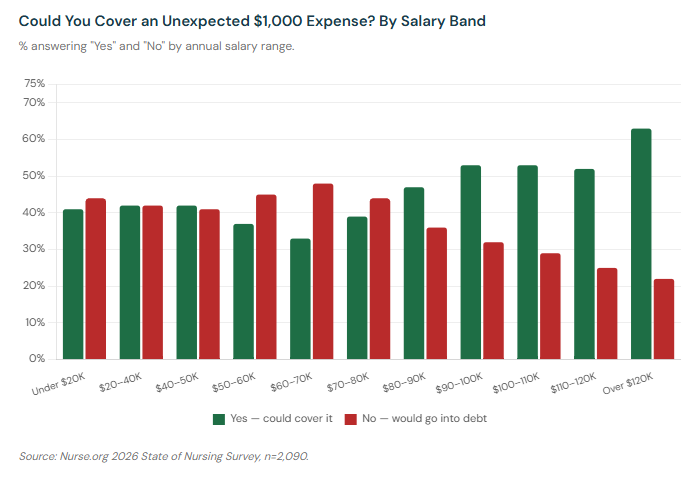
The education breakdown reveals a troubling gap between credential and compensation. LPN/LVNs — who make up 12% of our survey respondents — are among the most financially precarious: 53% say they could not cover a $1,000 emergency without debt, and many earn in salary bands where financial comfort is the exception rather than the rule. Nursing students currently working are similarly exposed, with 50% unable to cover the emergency.
The age pattern is more nuanced than expected. Nurses aged 40–54 — often mid-career, potentially carrying mortgage debt, supporting families, and at peak financial responsibility — show the highest rates of financial strain: between 44–47% in the 40–54 age range say they could not cover the $1,000 emergency. Nurses 65 and older show notably less strain (27% cannot cover it), which likely reflects paid-off mortgages, dual household incomes, and approaching or active retirement.
The mid-career squeeze deserves attention. These are often the nurses with the most clinical experience, the highest patient complexity they're managing, and the greatest potential departure risk. Their financial fragility is a retention problem as much as a compensation problem.
Working More to Get By
When nursing salaries don't stretch far enough, nurses find other ways to fill the gap. In our survey, financial stress drove a significant share of career decisions over the past 12 months:
- 37% worked extra shifts or overtime due to financial stress
- 15% took a second job due to financial stress
- 8% considered leaving bedside nursing due to financial stress
- 27% said financial stress has not affected their career decisions
More than a third of all nurses — 37% — said financial pressure pushed them to work extra shifts or overtime. This isn't a small or marginal group. It represents roughly 775 of the 2,090 nurses in our survey.
The overtime picture is particularly striking when broken down by salary. Nurses earning $70,000–$100,000 a year are the most likely to be working extra shifts due to financial stress — 42–47% in that band. This suggests that mid-range earners, not the lowest earners, feel the financial pinch most acutely in terms of behavior change. Nurses earning below $40,000 may already be in survival mode; nurses at $80,000–$90,000 are the ones closest to the threshold where they feel they should be financially stable — but aren't.
About 20% of nurses supplement their income with a secondary source. But most of that supplemental income comes from doing more nursing, not from building an independent income stream. The most common secondary income sources are overtime shifts (8%) and per diem work (7%). The profession itself is the safety net — and that safety net has limits.
- "Salaries that are not commensurate with inflation and lack of overtime availability — as a result of hospitals trying to save money — cause nurses to need to take a second job or a job with an agency. And agencies are not paying well either when you calculate housing cost away from home."
- "Since our community hospital has been bought out, our staffing and supplies are at an all-time shortage and our patient census and acuity is at an all-time high. I feel we are being pushed to do what is not humanly possible and not given the support we need. Salaries have not kept up with cost of living, and what once was a comfortable salary is extremely tight."
One particularly striking finding: among the 309 nurses who said they took a second job specifically because of financial stress, 51% still cannot cover a $1,000 emergency without debt. Taking a second job helped — but for half of those nurses, it still wasn't enough.
The Debt Question and the "Worth It" Calculation
Financial stress in nursing doesn't start on the first day of the job. For many nurses, it starts in nursing school. In our survey, 76% of respondents carried some form of educational debt to become a nurse. More than a third carried at least $25,000 in debt; 20% carried more than $50,000.
That debt burden shapes how nurses feel about the investment they made. Among nurses who never carried educational debt, 91% say their nursing education was worth it. Among nurses who carried more than $150,000 in debt, only 61% say the same — and 18% say it was not worth it, the highest "not worth it" rate of any group we measured.
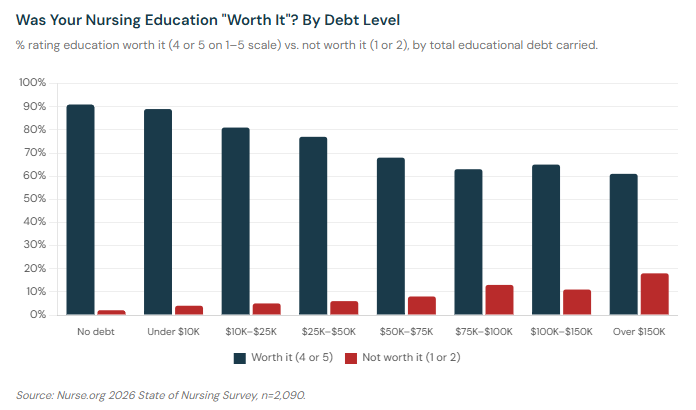
The declining "worth it" sentiment as debt increases reflects a real economic calculation. A nurse who borrowed $100,000 to earn a BSN and is now earning $75,000 a year — and cannot cover a $1,000 emergency — is not experiencing their education as a good investment. They're experiencing it as a debt trap.
- "Nurses continue to be overworked in unsafe staffing conditions, along with being underpaid with large amounts of school loan debt. On-the-job training for new grad nurses is too short because they often need you to work on your own ASAP due to inadequate staffing."
- "I feel like I am putting my license on the line every day for $200 a day. All in all I love nursing and would not change it — but nothing seems to change."
Benefits Are Eroding Too
Pay is only part of the compensation picture. Benefits — health insurance, retirement matching, paid time off — make up a significant share of total compensation for most nurses. And in our survey, 34% of nurses say their benefits got worse over the past year. Only 5% say their benefits improved.
That matters because when benefits erode, nurses effectively take a pay cut even if their base salary stays the same or goes up. A nurse who received a 3% raise but now pays higher health insurance premiums, lost their 401k match, or absorbed higher out-of-pocket deductibles may have ended the year in a worse position than the year before.
- "Constantly being asked to do more and more without any increase in compensation. We have to fight tooth and nail for cost-of-living raises, we lost our employer-sponsored health insurance and have to pay our own, we no longer get 401k employer matching. Meanwhile, the CMO got an $85,000 bonus."
- "Benefits are horrid. The new contract states we are not eligible for a raise for 3 years. Our health care coverage is now exorbitant and piecemeal. I am now 51 years old and I know I will never be able to retire."
The combination of modest salary increases, rising benefit costs, and persistent financial fragility creates a compound problem. Nurses are earning more on paper and falling further behind in practice. The headline numbers on nurse pay are improving. The lived experience of nurse finances, for a substantial portion of the workforce, is not.
What Nurses Are Saying
The comments nurses left in our survey on this topic were some of the most candid in the entire dataset. The same themes appeared consistently: raises that don't keep pace with costs, a sense that the profession demands everything and compensates accordingly little, and a workforce that is working extra to stay in place.
- "The nursing profession has become more stressful since I graduated school many years ago, but pay has not increased like it should. I do not believe that nurses with many years of experience are treated as though they are an asset for their organization."
- "After 48 years in nursing, I am still making the same amount of money I made 20 years ago. No compensation for inflation after you reach the top of the pay scale."
- "Nurses are underpaid for the amount of work and absolute perfection expected. CEOs draw a huge salary and massive bonus while we are consistently thrown into unsafe situations with inadequate staffing and lack of support. That's what our 'incentive-based' slap-in-the-face 1–2% raises are based on. It's disgusting."
- "Nursing has gotten harder with less pay. Hospital CEO/CFOs have only gotten bigger pockets. Our national healthcare system is severely broken. I have been a nurse for 46 years and it frightens me to think what my grandson will endure in the future of healthcare."
The financial picture in nursing is not one of a profession that can't attract competitive pay. It is one of a profession whose compensation has not kept pace with what it actually demands of its workforce — in hours, in risk, in physical and emotional cost — and where modest nominal pay increases are being quietly eaten by rising healthcare premiums, depleted retirement benefits, and the enduring weight of student debt.
Nurses are doing more. Their paychecks say they're earning more. The question the data forces is whether anyone with the power to change it is paying attention to the gap between those two facts.
This article is part of Nurse.org's ongoing coverage of the 2026 State of Nursing Survey.


